Interviews

A handy tool for easy, stress-free clinical examinations!
Naoki Ohmiya
Prof. Naoki Ohmiya (Chairman, Department of Gastroenterology, Fujita Health University) is developing a "magnetically-controlled whole gastrointestinal tract capsule endoscope"
Interviewer:Satoshi Endo、Author:Junko Kuboki、Translated by:FUJIYAMA, Co., Ltd.、Photography by:addingdesign LLC.

Is there no way to examine everything from the mouth to the esophagus, stomach, small intestine and through into the large intestine in a single go?
Endoscopic examinations are said to be the surest method of detecting cancer in the stomach, large intestines or other parts of the digestive tract by allowing for direct observation of the lesions. Endoscopy typically involves using one of two different types of endoscopes in the form of a tube that is inserted into the body: a gastroscope (a camera for observing the upper digestive tract) or a colonoscope (a camera for observing the large intestine). However, as this involves forcing a tube into a person’s mouth, nose or anus for internal observation, it can also be considered a somewhat barbaric form of medical examination.
“It is not a pleasant experience at all. I myself certainly do not care for it. If given the choice, I would definitely prefer not to undergo an endoscopic exam,” Dr. Ohmiya says with a laugh, “since I personally dislike it, I have been searching for a better way of doing things.”
Dr. Ohmiya is a seasoned gastroenterologist with extensive experience as a medical practitioner and researcher, but even he will gladly tell you that he does not care for gastroscopic exams. Is it any wonder, then, that a layperson might recoil at the mere mention of a gastroscope?
Recently, however, some new devices have come onto the scene. The “balloon endoscope” currently under development aims to overcome one of the main shortcomings of conventional endoscopes: the inability to enter the meandering small intestines, which expand and contract as though they had a mind of their own. Meanwhile, another new development is the “capsule endoscope,” which eschews the tube entirely in favor of a small capsule with a built-in camera that is swallowed and, ultimately, expelled through the anus.
A fan of the capsule endoscope, in particular, Dr. Ohmiya says, “It is great because it puts less stress on the body.” Capsule endoscopes were first developed by an Israeli company called Given Imaging (now Medtronic) in the year 2000 and approved for research use in Japan in 2004. Increasingly covered by insurance since 2007, capsule endoscopes are becoming more and more common in clinical settings. The first capsule endoscopes were developed for the small intestines, but versions for the large intestines soon followed.
Whenever he performed endoscopic exams, Dr. Ohmiya would often wonder to himself, “Why are there separate capsules for the small and large intestines? It seems like a waste to only examine one or the other after having a patient go to the trouble of swallowing a capsule. If only we could look at the mouth, esophagus, stomach, small intestines, large intestines and anus in a single go.”
The reason for this is the fact that conventional capsule endoscopes are unable to observe every section of the digestive tract in sufficient detail. Particularly with the esophagus and stomach, the capsule simply does not stay in one place long enough. Once swallowed, the capsule reaches the stomach in under two seconds. In the relatively spacious stomach, the capsule will soon roll down to the bottom, whereas a doctor would want to observe the cardiac sphincter (i.e. the entrance) and the upper areas of the stomach as well. Unlike a tube endoscope, a capsule is at the mercy of gravity and peristalsis, which inevitably leads to blind spots in observation.
“In short, the only way to really take full advantage of the merits of a capsule would be to control the position of the capsule from outside of the body. Of course, I am not the only person to think of this. In fact, medical equipment manufacturers are currently developing magnetic induction devices akin to an MRI. However, from a clinical perspective, such large-scale devices are simply not very practical. All a doctor really needs is a handy device that is easy to operate and allows the doctor to change the position of the capsule at will.”

The capsule endoscopes that Dr. Ohmiya uses are quite compact. Compared to gastroscopes and other tube endoscopes, these capsules put less stress on the bodies of patients. The challenge lies in finding a way for doctors to control the capsule at will.
Controlling a Conventional Capsule Endoscope with Magnets
And so, Dr. Ohmiya sought out the assistance of experts in the field of applied magnetics engineering: the researchers at the Tashiro Laboratory and the Mizuno Laboratory in the Department of Engineering at Shinshu University. The researchers initially thought of adding a magnet to the capsule to make it move, but a magnetic capsule would not be usable in clinical settings for quite some time. This is because making modifications or adding parts to a device that has already been approved for medical use is considered to be the same as developing an entirely new device, meaning that the resulting device must then be proven safe for use on humans. Dr. Ohmiya, therefore, requested a “device that could be used to control an already approved and readily available capsule.”
And so, the researchers turned their attention to the button battery inside of the capsule. With special processing and added strain, the battery’s stainless-steel enclosure could be magnetized thanks to a phenomenon called strain-induced Martensitic transformation. Thus, if a magnet could be designed to control the button battery through magnetic induction, then it might also be possible to control a capsule endoscope itself.
Through basic experimentation, the researchers found that controlling a capsule inside of the digestive tract from the surface of a human body would require a magnetic field with a strength of 17mT (milliTesla: a measure of magnetic flux density) at a distance of about 10cm when suspended in water. They considered using a device that relied on electromagnets, but such a device would also require some sort of cooling system, making it rather expensive. As Dr. Ohmiya and the researchers wanted to prioritize convenience and promote widespread use, they decided to use permanent magnets instead. Consequently, they set about adjusting the strength of the magnetic field through repeated fine-tuning of the layout of the magnets in the device.
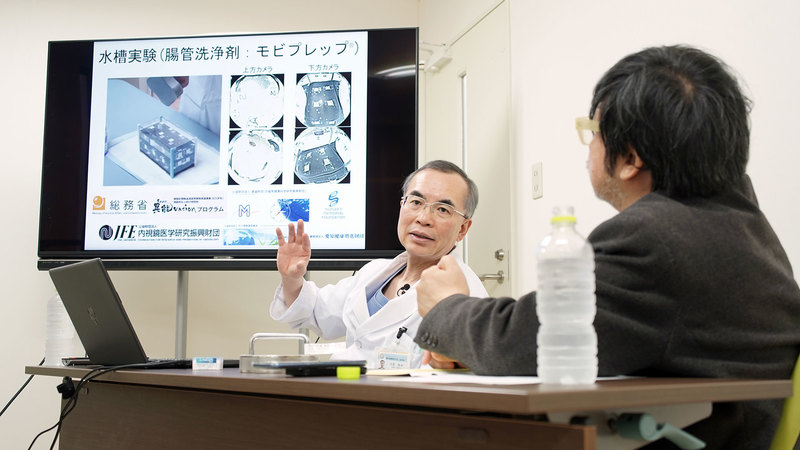
Explaining the experiments that were conducted in the early stages of development using a water tank. Although a battery is not originally intended to be used in this way, placing the material of a battery’s enclosure in a magnetic field allows the battery to be moved with a magnet.
Their back and forth communication and trial and error finally culminated in the “magnetically-controlled whole gastrointestinal tract endoscopic capsule” system. This simple and straightforward system involves pressing a handy tool against the body of a patient who has swallowed a capsule endoscope in order to guide the capsule through the patient’s body while also taking advantage of changes in posture.
When he first saw the imagery from a capsule inside of a patient’s stomach, Dr. Ohmiya was simply amazed. His first thought was, “Wow, I didn’t expect it to be like this!” With two cameras, the capsule provides a nearly 360° sweeping view of the lumen (i.e. cavities) of the digestive tract. In addition, unlike gastroscopes, which have tubes and shafts that can block the field of vision, the capsule is not attached to any tube, meaning that a doctor can observe the natural physiology of the lumen of the digestive tract without obstruction. One could even say that it feels like being an explorer venturing inside the body.
“Conventional tube endoscopes are inserted while air or carbon dioxide is pumped inside, which makes everything look like it has been flattened. By contrast, a capsule simply floats in water (actually a digestive tract cleanser), which makes lesions or flat polyps seem to stand out, making discovery more likely.”
The capsule size is about 11x31mm and it weighs just 5g. In order to ensure patient safety, each capsule is disposable and intended for single use. In the course of a single examination, it will take several hundred-thousand photographs.
With this system, because the capsule itself is controlled through magnetic induction, it is also possible to control how long it remains in the body. While a conventional capsule endoscope takes anywhere from a few hours to ten hours to pass through the body until expulsion, this system can shorten that time to under four hours (as it can be propelled forward in cases where constipation slows nature’s course).
One other issue is “interpretation” (i.e. arriving at a diagnosis based on analysis of endoscopic imagery). Dr. Ohmiya is already using this system in clinical trials to carefully examine actual patients, but even he takes 3 or 4 hours to interpret the imagery from a single patient. However, once whole digestive tract capsule endoscopy becomes common, Dr. Ohmiya believes that“automated AI-based diagnosis will be possible in the near future.”
Another major issue involves securing research funding. The actual cost of each capsule is some 70,000 yen. Plans for the future commercialization of this system require completion of the process for obtaining insurance coverage (i.e. ensuring that the device is covered by health insurance), but this will require more extensive clinical trials as well as multicenter studies. Obtaining clinical case studies from 100 patients alone requires a budget that ranges in the tens of million yen.
Undeterred, Dr. Ohmiya continues to push forward with his research. “By the end of 2020, I will have 100 case studies from the randomized sham-controlled comparative study* that I am currently working on. After that, I hope to move on to multicenter studies.” [*Note: This is a strictly controlled and highly evidence-based method of clinical testing intended to demonstrate the effectiveness of using this system as opposed to not using this system.]
Toward Providing Cancer Screenings for Countries with High Rates of Stomach Cancer in Asia & South America, for Countries with High Exam Costs in Europe & North America and Even for Children
Probably not many people outside of the medical field know this, but the prevalence of gastrointestinal cancers varies between races and regions. For example, a type of bacteria called Helicobacter pylori is a factor in stomach cancer, meaning this stomach cancer is more common in Asia and South America (where this type of bacteria is prevalent) than in Europe and North America (where it is not). The whole digestive tract capsule endoscopy system is already relatively inexpensive, but Dr. Ohmiya believes that, if the price comes down further, “It can do a lot of good for many people in regions of Asia and South America with high rates of stomach cancer.”
Meanwhile, there is little interest in stomach cancer screenings in Europe and North America, where stomach cancer rates are low. However, colon cancer is a major illness in these regions. As there is thus a need for colon cancer screenings, many manufacturers are actively engaged in the development of devices for this purpose (including capsule endoscopes). However, the inordinately high cost of screenings remains a major obstacle. This is because, in Europe and North America, endoscopy must be performed with an anesthesiologist present. With the introduction of a system that requires no anesthesia or special equipment, it might become easier for people in these regions to receive gastrointestinal endoscopy exams. Such a system would also allow people to receive exams in remote areas or sparsely populated islands, where it may be difficult to find a gastroenterologist, much less a facility equipped with endoscopes, CT scanners or fluoroscopes.

The themes that researchers choose to pursue are invariably influenced by their environments. There do not appear to have been any researchers in the western world who thought to extend the time that a capsule endoscope remains in a patient’s stomach.
In addition, Dr. Ohmiya says that this system could also be used to perform endoscopy on children. Because small children cannot easily swallow tube endoscopes, anesthesia is a necessity, which makes for tricky examinations. However, with a capsule of about 11x31mm, a child (age 10 or over) could swallow the capsule as though it were medicine. This system may very well be recognized as an effective examination method in the field of pediatrics as well.

Dr. Ohmiya’s endeavors to move a capsule endoscope with a permanent magnet are now ready for the biggest challenge of all: the clinical trials that lie ahead.
Whole GI tract capsule endoscopy has great potential for a wide range of applications: worldwide, regardless of racial background and even for children. However, there are still several more immediate challenges to overcome.
“I want to work with manufacturers to establish a production system for magnetic induction devices so that we can make them more affordable.” “In time, I also want to start negotiating with capsule endoscope manufacturers toward having magnets mounted inside of mass-produced capsules.” “Operating the device takes some getting used to, so there is also an urgent need to draft a manual on how to use it in examinations.” Even while he is busy working on clinical trials, Dr. Ohmiya is also looking into the challenges that lie ahead and thinking about how to overcome them.
The driving force behind his work is the inspiration that he drew from his actual experience of practicing medicine. It all started with his strong desire to discover lesions in patients as quickly as possible and to establish a cheap, inexpensive method of examining patients without putting undue stress on their bodies.
This system is much more than simply a tool for doctors to use. The cluster of magnets within the device holds the knowledge, experience and hard work of researchers who are at the forefront of their respective fields, as well as the futures of many people whose lives depend on the discovery of tiny lesions inside of their bodies.
Naoki Ohmiya M.D., Ph.D., AGAF.
He received his M.D. in 1988, and his Ph.D. in 1995. He was a research fellow at The Burnham Institute (San Diego, California) in 1997-8, an assistant and associate professor at the Department of Gastroenterology and Hepatology, Nagoya University Hospital in 2001-13, an associate professor at the Department of Gastroenterology, Fujita Health University in 2013-2015. He has been a professor and chairman of the Department of Gastroenterology at Fujita Health University. His research fields include endoscopic diagnosis and treatment of gastroduodenal diseases, capsule endoscopies, small bowel diseases, inflammatory bowel disease, fecal microbiota transplantation, molecular mechanisms of carcinogenesis in the alimentary tract, and biomarker development of gastrointestinal tumors.

